Translate this page into:
Efficacy of microneedling with platelet-rich plasma versus microneedling with tranexamic acid in melasma – A randomized open-label study
*Corresponding author: Rashmi Sarkar, Department of Dermatology, Lady Hardinge Medical College, New Delhi, India. rashmisarkar@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Jain A, Sarkar R, Mendiratta V, Garg T, Meena AK. Efficacy of microneedling with platelet-rich plasma versus microneedling with tranexamic acid in melasma – A randomized open-label study. J Cutan Aesthet Surg. doi: 10.25259/JCAS_48_2024
Abstract
Objectives
Melasma is a recalcitrant hyperpigmentary disorder requiring innovative treatment options for its management. The objectives of the study are to compare the efficacy of microneedling with platelet-rich plasma (PRP) versus microneedling with tranexamic acid (TXA) in melasma in terms of Modified Melasma Area and Severity Index Score (mMASI), Physician Assessment Score (PAS), and Patient Satisfaction Score (PSS) among them.
Material and Methods
This was a randomized open-label study in which 50 cases of melasma (18–60 years) were included. Patients were randomly allocated into 2 groups of 25 patients each. Group 1 was treated with microneedling with PRP and group 2 with microneedling with TXA for three sessions every 3 weeks, and were followed up till 15 weeks.
Results
Mean mMASI decreased significantly from 7.14 to 3.88 and 7.65 to 4.24 in groups 1 and 2, respectively, from baseline to 15 weeks (P < 0.001) and statistically significantly between the 2 groups (P = 0.043). However, no significant difference was found between PAS and PSS between them.
Conclusion
Microneedling was found to be effective with both PRP and TXA in melasma. However, microneedling with PRP demonstrated greater efficacy versus TXA. Hence, it can be considered a promising treatment modality in the future.
Keywords
Melasma
Microneedling
Platelet-rich plasma
Tranexamic acid
INTRODUCTION
Melasma, an acquired hypermelanosis, is characterized by bilateral, brown-colored macules on sun-exposed areas of skin, more prevalent in middle-aged females.1 To date, the pathogenesis of melasma has not been fully elucidated; however, chronic ultraviolet (UV) exposure, female hormonal stimulation, thyroid dysfunction, and genetic background have all been proposed to be the predisposing factors.2
The management of melasma is an ongoing challenge. Conventional treatment includes sunscreen and depigmenting agents, often in combination with other therapies, such as topical tretinoin, corticosteroids, or superficial peeling agents.3 Even after treatment, skin discoloration may not always disappear completely and each patient may have to try various treatment options to achieve satisfactory results.
Newer treatment options include microneedling alone or in combination with platelet-rich plasma (PRP)/tranexamic acid (TXA). Microneedling acts by creating thousands of microchannels that act as a stimulus for wound healing. This induces matrix metalloproteinases, which are thought to reduce hyperpigmentation.4 PRP contains various growth factors and cytokines that stimulate various effects in soft tissue. It could be a promising treatment option with reduced chances of rebound hyperpigmentation relative to other treatment options.5,6 Tranexamic acid acts by inhibiting plasminogen-keratinocyte interaction by decreasing the tyrosinase activity, causing decreased melanin synthesis from melanocytes.7
The main aim of the study was to compare the efficacy of microneedling with PRP and microneedling with TXA in melasma in terms of Modified Melasma Area and Severity Index Score (mMASI), Physician Assessment Score (PAS), and Patient Satisfaction Score (PSS) among two groups.
MATERIAL AND METHODS
This randomized open-label study was conducted from November 2022 to February 2024 in the Dermatology outpatient department of a tertiary care center in North India. A total of 50 adult clinically diagnosed cases of melasma with ages ranging from 18 to 60 years were included. Pregnant and lactating women, patients with a history of any treatment for melasma in the past 1 month, active infection over the face, and known case/history suggestive of coagulation or bleeding disorders were excluded. Institutional Ethics Committee approval was granted before starting the study. Patients were allocated into two groups, consisting of 25 patients each. In Group 1, microneedling was done, followed by topical application of PRP, while in Group 2, microneedling was done, followed by 10% TXA application every 3 weeks for 3 sessions.
A detailed history, including site of onset, duration, history of drug intake, and family history, was taken. All subjects were examined in detail for type and morphology and were also subjected to dermoscopic examination using DermLite DL4. Pre- and post-treatment photographs were taken.
PRP was prepared using the double spin method. Microneedling was done using a derma roller containing microneedles of size 1 mm (10 passes in each direction). The treatment endpoint was uniform pinpoint bleeding. Following this, PRP/TXA was topically applied over the treated area. The improvement in melasma was assessed using mMASI scoring at baseline and before each session. This score was calculated as follows:
It includes two factors: Area of involvement (A) and Darkness (D). These are assessed in four areas, including forehead (f) 30%, right malar (rm) 30%, left malar (lm) 30%, and chin (c) 10%. Area of involvement is given the numerical values as follows: 0 = No involvement, 1 = <10%, 2 = 10–29%, 3 = 30– 49%, 4 = 50–69%, 5 = 70–89%, and 6 = 90–100%. Darkness is rated on a scale from 0 to 4 as Absent (0), slight (1), mild (2), marked (3), and maximum (4).
Modified MASI = 0.3 A(f) D(f) + 0.3 A(rm) D(rm) + 0.3 A(lm) D(lm) + 0.1 A(c) D(c)8
The PAS was calculated using photographs at baseline and then after each session. The photographs were compared and evaluated independently by an observer using a 5-point scale for improvement as follows: No improvement (0), 1–25% (1), 26–50% (2), 51–75% (3), 76–100% (4). The PSS was calculated as follows: Worsening (−1), no improvement (0), mild improvement (1), moderate improvement (2), and excellent improvement (3). Three sessions at 3 weekly intervals were done with subsequent follow-up visits at 9 weeks, 12 weeks, and 15 weeks.
The data collected was entered into a Microsoft Excel spreadsheet and was analyzed using the Statistical Package for the Social Sciences software version 23. Continuous variables were expressed as mean ± standard deviation and were analyzed using a t-test. Categorical variables were expressed as frequencies and percentages and were analyzed using the Chi-square test. Other appropriate tests, such as the Wilcoxon–Mann–Whitney test and generalized estimation equations method, were applied wherever applicable. Statistical significance was assumed at a P < 0.05.
RESULTS
A total of 50 cases of melasma (18–60 years) were recruited in this study. The age ranged from 25–45 years with the mean age being 32.94 ± 5.08 years. Most of the patients (52%) were in the age group of 31–40 years, followed by 21–30 years (40.0%) and 41–50 years (8.0%). The majority of the patients were females (86%). Dermoscopy was done in all to classify them into epidermal, dermal, and mixed melasma. Clinicoepidemiological features and dermoscopic findings observed in our study are depicted in Table 1.
| Characteristics | Number (%) |
|---|---|
| Gender | |
| Females | 43 (86) |
| Males | 7 (14) |
| Occupation | |
| Homemaker | 36 (72) |
| Government job | 5 (10) |
| Cook | 3 (6) |
| Teacher | 2 (4) |
| Parlor | 1 (2) |
| Tailor | 1 (2) |
| Textile shop | 1 (2) |
| Hair stylist | 1 (2) |
| Sites involved at present | |
| Cheeks | 50 (100) |
| Nose | 33 (66) |
| Forehead | 18 (36) |
| Upper lip | 12 (24) |
| Chin | 5 (10) |
| Mandible | 4 (8) |
| History of drug intake (OCPs) | |
| Present | 10 (20) |
| Absent | 40 (80) |
| Family history | |
| Present | 15 (30) |
| Obstetric history | |
| Nulligravida | 1 (2) |
| History of single pregnancy | 9 (18) |
| History of multiple pregnancies | 31 (62) |
| Onset of melasma during gestation | |
| Total | 8 (20) |
| First trimester | 5 (62.5) |
| Second trimester | 2 (25) |
| Third trimester | 1 (12.5) |
| Triggering factors | |
| Occupation (homemakers) | 36 (72 |
| History of sun exposure (>1 h) | 38 (76 |
| OCPs intake | 10 (20) |
| History of thyroid disorder | 3 (6) |
| History of multiple pregnancies | 31 (62) |
| Type of melasma | |
| Centrofacial | 41 (82) |
| Malar | 9 (18) |
| Type of melasma on the basis of dermoscopy | |
| Epidermal | 24 (48) |
| Mixed | 16 (32) |
| Dermal | 10 (20 |
| Dermoscopic findings | |
| Sparing of follicles and sweat gland openings | 41 (82) |
| Brown dots/globules/granules | 37 (74) |
| Regular pigment network | 25 (50) |
| Irregular pigment network | 9 (18 |
| Arcuate/annular structures | 7 (14) |
| Telangiectasia | 6 (12) |
| Irregular pattern | (12) |
| Serpentine lines | 4 (8) |
| Circles | 2 (4) |
| Straight lines | 2 (4) |
OCPs: Oral contraceptive pills
Mean mMASI decreased from 7.14 to 3.88 and 7.65 to 4.24 in group 1 and group 2, respectively, from baseline to 15 weeks. This change was statistically significant (P < 0.001) in both the groups. Table 2 depicts the comparison of the change in mean mMASI in both groups over time.
| mMASI | Group | P-value for comparison of the two groups at each of the timepoints (Wilcoxon–Mann–Whitney Test) | |
|---|---|---|---|
| PRP | TXA | ||
| Mean (SD) | Mean (SD) | ||
| Baseline | 7.14 (2.33) | 7.65 (2.91) | 0.954 |
| 3 weeks | 5.38 (2.12) | 6.17 (2.67) | 0.443 |
| 9 weeks | 3.88 (1.45) | 4.24 (1.71) | 0.655 |
| 15 weeks | 3.88 (1.45) | 4.24 (1.71) | 0.734 |
| P-value for change in mMASI over time within each group (Friedman test) | <0.001 | <0.001 | |
| Overall P-value for comparison of change in mMASI over time between the two groups (generalized estimating equations) | 0.043 | ||
mMASI: Modified melasma area and severity index score, PRP: Platelet-rich plasma, TXA: Tranexamic acid, SD: Standard deviation
The overall change in mean mMASI was compared between both groups and was found to be statistically significant (P = 0.043), with PRP giving better results than TXA in terms of mMASI.
The comparison of PAS and PSS in both groups at different time points is mentioned in Table 3. The scores calculated during each session were not influenced by the previous session. Hence, it indicates improvement only within each session rather than cumulative progress over time (P = 0.690 for PAS and 0.478 for PSS). Figures 1 and 2 depicts improvement in melasma from baseline till 9th week in patients treated with microneedling with PRP and microneedling with TXA group respectively. Hence, the overall change in PAS and PSS between the groups was found to be non-significant. In group 1, a total of 16 patients (64%) experienced adverse effects out of which 14 (56%) reported erythema and 2 (8%) reported pain. While in group 2, a total of 12 patients (48%) reported adverse effects of which 9 (36%) developed erythema and 3 (12%) reported pain.
| PAS | Group | P-value for comparison of the two groups at each of the timepoints (Wilcoxon–Mann–Whitney Test) | |
| PRP | TXA | ||
| Mean (SD) | Mean (SD) | ||
| 3 weeks | 1.40 (0.58) | 1.52 (0.59) | 0.435 |
| 9 weeks | 0.44 (0.65) | 0.48 (0.51) | 0.575 |
| 15 weeks | 0.00 (0.00) | 0.00 (0.00) | - |
| Overall P-value for comparison of change in PAS between both the groups | 0.690 | ||
| PSS | Group | P-value for comparison of the two groups at each of the timepoints (Wilcoxon–Mann–Whitney Test) | |
| PRP | TXA | ||
| Mean (SD) | Mean (SD) | ||
| 3 weeks | 1.00 (0.41) | 1.28 (0.68) | 0.063 |
| 9 weeks | 0.44 (0.51) | 0.44 (0.51) | 1.000 |
| 15 weeks | −0.04 (0.20) | 0.00 (0.00) | 0.337 |
| Overall P-value for comparison of change in PSS between both the group | 0.478 | ||
PRP: Platelet-rich plasma, TXA: Tranexamic acid, SD: Standard deviation, PAS: Physician assessment score, PSS: Patient satisfaction score
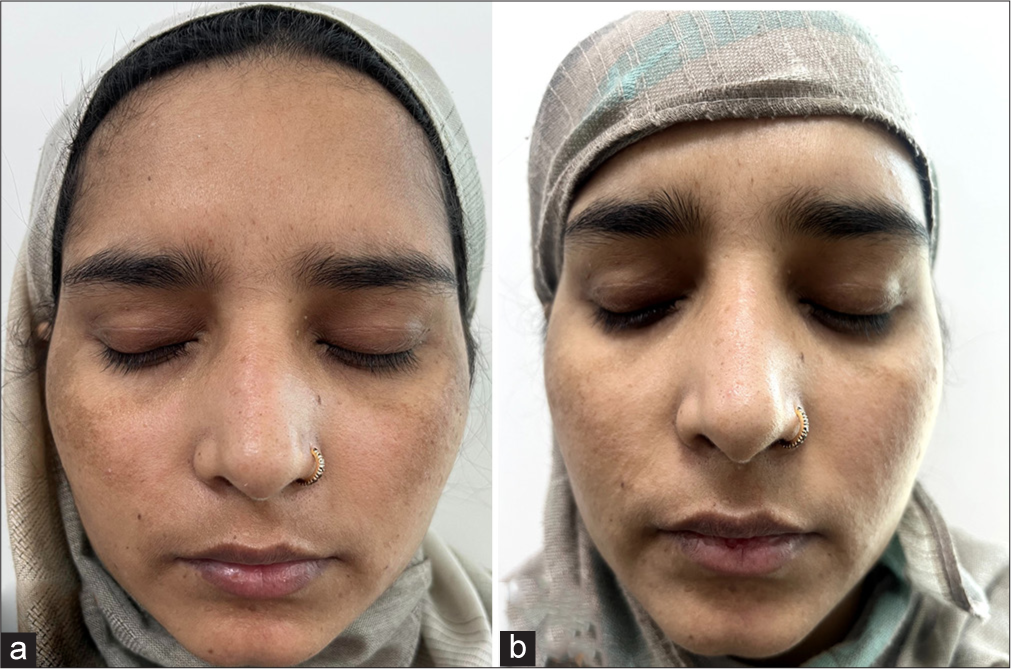
- (a) Global photographs at baseline of patient in microneedling with platelet-rich plasma (PRP) group. (b) Global photographs at 9th week of patient in microneedling with PRP group with improvement in melasma.
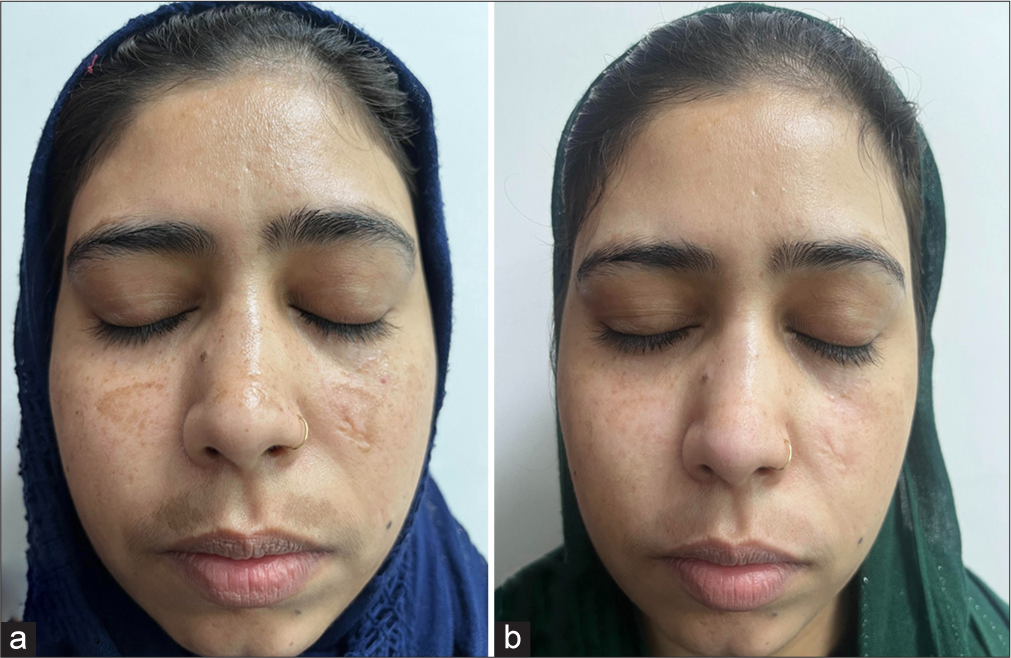
- (a) Global photographs at baseline of patient in microneedling with tranexamic acid (TXA group). (Patient has a scar from before). (b) Global photographs at 9th week of patient in microneedling with TXA group with improvement in melasma.
Furthermore, the epidermal type of melasma responded better as compared to the mixed and dermal type. The baseline mean mMASI of epidermal, mixed, and dermal melasma was 6.7, 7.3, and 7.9 and at 15 weeks, it decreased to 3.27, 3.9, and 5.8, respectively. The percentage change in mean mMASI observed in epidermal, mixed, and dermal melasma was 51.19%, 46.57%, and 26.58%, respectively.
DISCUSSION
A total of 50 cases of melasma were recruited. The mean age of patients in a multicentric cross-sectional study from India by Sarkar et al.9 was 38.02 ± 10.82 years. It was slightly higher as compared to our study, which may be due to the multicentric nature of their study as compared to our study, which was a single-center study. In a study by Guinot et al.,10 most common age groups affected were 30–39 years, which is similar to our study.
Maximum patients were homemakers (72%), followed by government workers (10%), cooks (6%), and teachers (4%). In congruence with our findings, another study from India reported predominantly homemakers (53.9%) among the patient cohort, wherein a notable correlation between cooking/occupational heat exposure and the severity of melasma was established.9 The potential impact of infrared and visible light spectrum remains an unexplored aspect necessitating further research in this area.
A family history of melasma was present in 30% of patients in our study. Hexsel et al.11 in a study from Brazil, reported a significant correlation between age of onset and positive family history of melasma. This probably indicates a potential genetic predisposition in melasma development.
Out of 41 married females, 62% had a history of multiple pregnancies, followed by single pregnancy and nulliparous in our study. Approximately 51% of women had a history of multiple pregnancies, followed by single pregnancy and no pregnancy, in a study from India.12 The prevalence of melasma onset during pregnancy ranges from 15% to 22%. Our results were also in this range.9,13,14 Therefore, pregnancy is indeed considered a contributing factor in melasma, as hormonal changes during pregnancy can trigger/exacerbate the condition.
Newer treatment options include microneedling, PRP, and TXA. These have been tried in many studies with variable responses individually as well as in combination with each other. Microneedling is a minimally invasive procedure involving superficial and controlled puncturing of the skin by rolling with miniature fine needles. It acts by following mechanisms: (1) Increasing transcutaneous delivery of topical agents through microchannels,15,16 (2) microinjuries which lead to setting up a wound healing cascade with the release of various growth factors resulting in increased synthesis of elastin and collagen,17 and (3) increases transcutaneous elimination of melanin.18 Microneedling may be combined with other treatment modalities like PRP or TXA. Combination therapy yields superior outcomes as compared to standalone therapies due to enhanced penetration of PRP/TXA following microneedling.
The PRP has emerged as a new treatment modality for several dermatological and esthetic indications.19,20 The rationale behind using PRP in melasma is that upon activation of platelets, multiple growth factors are released, which stimulate the production of epidermal cells and fibroblasts, promote blood vessel formation, and induce collagen synthesis.21 Transforming growth factor-β1 downregulates the microphthalmia-associated transcription factor promoter and paired box 3, which ultimately leads to a reduction in the production of tyrosinase-related protein 1, tyrosinase, and tyrosinase-related protein 2. Epidermal growth factor also plays a role by inhibiting prostaglandin E2 expression and tyrosinase enzyme activity, thus lowering melanin production.
In our study, in group 1, mean mMASI decreased from 7.14 at the baseline to a minimum of 3.88 at 9 weeks (total duration of therapy) and remained constant at 12 and 15 weeks. This change in mean mMASI from baseline to 15 weeks timepoint was statistically significant (P < 0.001). Microneedling with PRP has been utilized for treating melasma in both Indian and international settings with variable response. A systematic review on PRP in melasma by Sarkar and Gupta22 analyzed 7 studies utilizing intradermal injections and microneedling for delivery of PRP, yielding good therapeutic outcomes in melasma. In another study by Hofny et al.6, 23 melasma patients were recruited, wherein PRP was delivered using microneedling (dermapen) on the right side of the face and intradermal injections were given on the left side for a total of 3 sessions every month. The mMASI decreased significantly from 5.71 ± 2.56 to 2.90 ± 2.05 after 3 sessions. Although a slightly better response was observed with microneedling, the difference between the two was not statistically significant. Microneedling delivered PRP more evenly and to a greater depth as compared to intradermal injection which may be responsible for better improvement in the microneedling group.
Similar to our study, the above-mentioned studies have also shown a significant reduction in the scores, mirroring our findings. This lends credence to the notion that a combination of microneedling and PRP may emerge as a future therapeutic option for managing melasma.
Tranexamic acid acts by inhibiting UV-induced plasmin activity in keratinocytes by blocking the binding of plasminogen to keratinocytes, thereby decreasing the production of prostaglandins, which are known stimulators of tyrosinase activity.23 For group 2, a significant decrease was noted in mean mMASI from 7.65 at baseline to a minimum of 4.24 at 9 weeks, which remained constant at 12 and 15 weeks (P < 0.001). Kaur et al.24 conducted a split-face, randomized, open-label study on 40 melasma patients, wherein microneedling was done on both sides, followed by 10% TXA solution on one side of the face (test side) and distilled water on the other side (control) at 2 weekly intervals till 6 weeks. Mean mMASI decreased from 4.313 ± 1.7781 to 1.471 ± 1.1242 and 3.899 ± 1.9641 to 3.090 ± 1.6648 in the test and control group, respectively. This decline was statistically significant (P < 0.05) within the groups. Another split face study by Ebrahim et al.25 from Egypt was done on 56 female patients with melasma. All patients received intradermal injections of TXA on one side of the face and microneedling with topical TXA on the other half every 2 weeks for a total of 6 sessions. There was a significant improvement in mMASI score from 13.83 ± 7.23 to 3.49 ± 2.91 on the injected side and from 13.83 ± 7.23 to 3.65 ± 2.32 on the microneedling side (P < 0.001). Although the decrease was significant on both sides individually, there was no statistically significant difference between both treated sides (P > 0.05). The results seen in other studies were in concordance with our findings, emphasizing the emerging role of the combination of microneedling with TXA in melasma.
While comparing the results between the two groups in our study, it was found that overall change in mMASI over time was statistically significant between both the two groups (P = 0.043), with microneedling with PRP giving better results than microneedling with TXA. To the best of our knowledge, only one similar study has been conducted so far by Gharib et al.26 in 2021 in Egypt. This study compared the therapeutic efficacy of microneedling with PRP versus microneedling with TXA in 26 melasma patients (13 patients in each group). Every patient was given four sessions every 4 weeks. According to the percentage change in MASI, a 50% improvement was noticed in the PRP group as compared to 42% in the TXA group from baseline to end of all sessions. When both groups were compared, the mean difference in MASI scores was statistically significant at the completion of the fourth session (P < 0.017), with PRP demonstrating superior results as compared to TXA, which is consistent with our findings (P < 0.043).
The comparison of overall change between two groups in terms of PAS did not yield any significant difference. To the best of our knowledge, no study directly compares PAS or photographic evaluations between PRP and TXA groups.
The overall change in PSS over time was compared, and no significant difference was found between the two groups (P = 0.478), which is similar to a study by Gharib et al.26 All side effects were mild in nature and self-resolving and did not require discontinuation of the treatment.
To the best of our knowledge, this is the first study from India that compared the therapeutic efficacy of microneedling with PRP versus microneedling with TXA in melasma. Limitations of our study include short-term follow-up of patients.
CONCLUSION
Management of melasma requires the exploration of innovative treatment options because of its chronic and resistant nature. In our study, both microneedling with PRP and microneedling with TXA were found to be effective in the management of melasma. Hence, both these treatment options can be used in the management of melasma as these therapies are effective and have minimum side effects. However, microneedling with PRP has shown better efficacy as compared to microneedling with TXA. We, therefore, recommend the use of microneedling with PRP as compared to microneedling with TXA. However, larger prospective randomized controlled trials with long-term follow-up are needed to reiterate further and establish the efficacy and safety of these modalities in the management of melasma.
Authors’ contributions
Ashna Jain - Concept, design, literature search, data analysis, data acquisition, drafting the article, manuscript editing, manuscript review, manuscript preparation, final approval of the version to be published. Rashmi Sarkar - Concept, design, literature search, data acquisition, manuscript editing, manuscript review, manuscript preparation, final approval of the version to be published. Vibhu Mendiratta - Concept, design, manuscript review, manuscript preparation, final approval of the version to be published. Taru Garg - Concept, design, manuscript review, manuscript preparation, final approval of the version to be published. Amit Kumar Meena -Concept, design, manuscript review, manuscript preparation, final approval of the version to be published.
Ethical approval
The research/study was approved by the Institutional Review Board at Lady Hardinge Medical College, number LHMC/EC/2022/PG Thesis/11, dated September 27, 2022.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.
References
- A melanosis of the face ("chloasma") Arch Dermatol. 1961;83:284-99.
- [CrossRef] [PubMed] [Google Scholar]
- Melasma: A comprehensive update: Part II. J Am Acad Dermatol. 2011;65:699-714.
- [CrossRef] [PubMed] [Google Scholar]
- Microneedling: A review and practical guide. Dermatol Surg. 2018;44:397-404.
- [CrossRef] [PubMed] [Google Scholar]
- Platelet-rich plasma is a useful therapeutic option in melasma. J Dermatolog Treat. 2019;30:396-401.
- [CrossRef] [PubMed] [Google Scholar]
- Efficacy and safety of tranexamic acid in melasma: A meta-analysis and systematic review. Acta Derm Venereol. 2017;97:776-81.
- [CrossRef] [PubMed] [Google Scholar]
- Reliability assessment and validation of the melasma area and severity index (MASI) and a new modified MASI scoring method. J Am Acad Dermatol. 2011;64:78-83, 83.e1-2
- [CrossRef] [PubMed] [Google Scholar]
- Clinical and epidemiologic features of melasma: A multicentric cross-sectional study from India. Int J Dermatol. 2019;58:1305-10.
- [CrossRef] [PubMed] [Google Scholar]
- Aggravating factors for melasma: A prospective study in 197 Tunisian patients. J Eur Acad Dermatol Venereol. 2010;24:1060-9.
- [CrossRef] [PubMed] [Google Scholar]
- Epidemiology of melasma in Brazilian patients: A multicenter study. Int J Dermatol. 2014;53:440-4.
- [CrossRef] [PubMed] [Google Scholar]
- A cross-sectional, multicentric clinico-epidemiological study of melasma in India. Dermatol Ther (Heidelb). 2014;4:71-8.
- [CrossRef] [PubMed] [Google Scholar]
- A global survey of the role of ultraviolet radiation and hormonal influences in the development of melasma. J Eur Acad Dermatol Venereol. 2009;23:1254-62.
- [CrossRef] [PubMed] [Google Scholar]
- Transcriptional profiling shows altered expression of Wnt pathway-and lipid metabolism-related genes as well as melanogenesis-related genes in melasma. J Invest Dermatol. 2011;131:1692-700.
- [CrossRef] [PubMed] [Google Scholar]
- Microneedling in skin of color: A review of uses and efficacy. J Am Acad Dermatol. 2016;74:348-55.
- [CrossRef] [PubMed] [Google Scholar]
- Percutaneous collagen induction: An effective and safe treatment for post-acne scarring in different skin phototypes. J Dermatolog Treat. 2014;25:147-52.
- [CrossRef] [PubMed] [Google Scholar]
- Early clinical and histological changes induced by microneedling in facial melasma: A pilot study. Indian J Dermatol Venereol Leprol. 2019;85:638-41.
- [CrossRef] [PubMed] [Google Scholar]
- A face-split study to evaluate the effects of microneedle radiofrequency with q-switched Nd: YAG laser for the treatment of melasma. Ann Dermatol. 2019;31:133-8.
- [CrossRef] [PubMed] [Google Scholar]
- Can platelet-rich plasma be used for skin rejuvenation? Evaluation of effects of platelet-rich plasma on human dermal fibroblast. Ann Dermatol. 2011;23:424-31.
- [CrossRef] [PubMed] [Google Scholar]
- Treatment of periorbital hyperpigmentation using platelet-rich plasma injections. Am J Dermatol Venereol. 2014;3:87-94.
- [Google Scholar]
- Inhibition of PAX3 by TGF-beta modulates melanocyte viability. Mol Cell. 2008;32:554-63.
- [CrossRef] [PubMed] [Google Scholar]
- Platelet-rich plasma in melasma-a systematic review. Dermatol Surg. 2022;48:131-4.
- [CrossRef] [PubMed] [Google Scholar]
- Tranexamic acid can treat ultraviolet radiation-induced pigmentation in guinea pigs. Eur J Dermatol. 2010;20:289-92.
- [CrossRef] [PubMed] [Google Scholar]
- Clinical efficacy of topical tranexamic acid with microneedling in melasma. Dermatol Surg. 2020;46:e96-101.
- [CrossRef] [PubMed] [Google Scholar]
- Tranexamic acid for melasma treatment: A split-face study. Dermatol Surg. 2020;46:e102-7.
- [CrossRef] [PubMed] [Google Scholar]
- Therapeutic effect of microneedling with platelet-rich plasma versus microneedling with tranexamic acid for melasma. J Clin Aesthet Dermatol. 2021;14:44-8.
- [Google Scholar]






