Translate this page into:
In the face of a rare foe: Aggressive angiomyxoma of the vulva – A case report and literature review
*Corresponding author: Charu Sharma Department of Obstetrics and Gynecology, All India Institute of Medical Sciences, Jodhpur, Rajasthan, India. sharma.charu651@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Kumar R, Shekhar S, Sharma C, Rao M, Patra S, Singh P. In the face of a rare foe: Aggressive angiomyxoma of the vulva – A case report and literature review. J Cutan Aesthet Surg. doi: 10.25259/jcas_26_24
Abstract
Angiomyxoma is a rare, benign mesenchymal tumor that predominantly occurs in the pelvic and perineal regions. This case report presents a unique instance of 7 × 5 cm angiomyxoma (AM) arising in the vulvar region. The patient underwent an incisional biopsy followed by a wide local excision. Histopathological examination and immunohistochemical staining confirmed the mesenchymal origin of the tumor. Follow-up examinations demonstrated no recurrence after 1 year of follow-up. This case highlights the rarity of vulvar AM and emphasizes the importance of considering such tumors in the differential diagnosis of vulvar masses. The discussion encompasses the clinical presentation, diagnostic challenges, and treatment modalities associated with vulvar AM, contributing to the existing literature on this infrequent entity.
Keywords
Angiomyxoma
Myxoid
Spindle
Vulva
Wide local excision
INTRODUCTION
Aggressive angiomyxoma (AAM) of the vulva is an extremely rare, benign, locally invasive and slow-growing mesenchymal tumor. Only about 350 cases of this condition are reported in the literature. In 1983, Steeper and Rosai were the first to describe this particular entity.1 This enigmatic tumor exhibits a distinctive histopathological pattern and poses considerable diagnostic and therapeutic challenges due to its unusual presentation and unpredictable clinical course. It arises from the myxoid cells of the connective tissue. This tumor is more common among females of reproductive age, with a male-to-female ratio of 1:6.6.2
Women usually present with a large perineal solid growth, which is usually multilocular polypoidal swelling with solid consistency. It involves the pelvis, perineum, vulva, vagina, and bladder. It may resemble warts, Bartholin duct cysts, lipomas, vulval abscesses, Gartner’s duct cysts, vaginal cysts, and prolapses, and the rarity of the tumor makes it difficult to diagnose at an early stage.3 Microscopically, AAM is characterized by its hypocellular and myxoid stroma, interspersed with thin-walled blood vessels. It is well known for high local recurrence, hence named as aggressive but with less metastatic potential. The tumor’s infiltrative growth pattern makes complete surgical resection challenging, often leading to the persistence or recurrence of the disease. Various clinicians have tried adjuvant hormonal therapy in the form of gonadotropin -releasing hormone (GnRH) agonists and aromatase inhibitors to prevent recurrence and showed promising results, but these therapies require more extensive research to make them a standard point of care. Clinicians and pathologists alike must be vigilant in distinguishing AAM from other mesenchymal tumors to guide appropriate management strategies.
The purpose of this case report is to gain a better understanding of the behavior of AAM, guide the surgeons to have clinical suspicion, and carry out meticulous radicalization to prevent a recurrence.
CASE REPORT
We report a case of a 20-year-old unmarried female who presented with the only complaint of swelling over the perineum for the past 1 year. Initially, the growth was of pea size and gradually increased to the present size in 1 year. There was no significant medical or family history. The patient was of average build with no signs of systemic illness, and her menstrual cycles were regular with average blood flow. During the local examination, a 7 × 5 cm painless solid growth was observed on the left labia minora with a polypoidal surface. There was no discharge or ulceration, and the contralateral labia appeared normal [Figure 1]. Inguinal lymph nodes were not enlarged, and there were no signs suggestive of perineal infection. In addition, the patient’s blood investigations and abdominal ultrasound showed no abnormalities. An incisional biopsy was performed, and the histopathological examination (HPE) showed a hypocellular lesion with diffuse loose myxomatous stroma containing fibrillar collagen and bland spindled to stellate-shaped cells. These findings were suggestive of angiomyxoma (AM) [Figure 2]. Wide local excision of the tumor was performed under anesthesia, and the labia was reconstructed. HPE showed skin and a tumor in the deep dermis and subcutis with ill-defined borders. The tumor was hypocellular and was composed of diffuse myxoid to edematous stroma with a few interspersed monomorphic to mildly pleomorphic spindled to stellate cells with delicate cytoplasmic processes, bland nucleus, and inconspicuous nucleoli. No lobules were seen, and no cytological atypia, mitosis, or necrosis were seen in the sections examined. Interspersed thin-walled and thick-walled vessels were seen within the tumor. A few vessels showed perivascular condensation of smooth muscle and fibrillary collagen. On immunohistochemistry, the tumor cells were positive for CD34, estrogen receptor (ER), and progesterone receptor (PR) [Figure 3] and were focally positive for desmin and smooth muscle actin. The tumor cells were negative for myogenin, panCK, and S100-P. Overall features confirmed the morphological diagnosis of AAM. Her post-operative recovery was uneventful. The patient was advised to follow-up every 2–4 months for clinical examination. No recurrence was noted on the ipsilateral side after 1 completed year of follow-up. However, a novel growth of 2 × 2 cm was seen arising from the right labia majora with similar characteristics.

- (a) Arrow shows the pre-operative image of pedunculated growth on left labia and (b) post-operative image after 4 months.
![(a) Scanner view showing epidermis (partially encircled with red in the upper right corner), and a myxoid tumor in the deep dermis, marked with black arrow (hematoxylin and eosin [H&E], ×20); (b) low-power view showing a hypocellular lesion with diffuse loose myxomatous stroma and interspersed thick-walled and thin-walled vessels. (H&E, ×10); (c and d) high-power view showing a hypocellular lesion with diffuse loose myxomatous stroma containing fibrillar collagen and bland spindled to stellate-shaped cells (H&E, ×40).](/content/173/2025/0/1/img/JCAS-26-24-g002.png)
- (a) Scanner view showing epidermis (partially encircled with red in the upper right corner), and a myxoid tumor in the deep dermis, marked with black arrow (hematoxylin and eosin [H&E], ×20); (b) low-power view showing a hypocellular lesion with diffuse loose myxomatous stroma and interspersed thick-walled and thin-walled vessels. (H&E, ×10); (c and d) high-power view showing a hypocellular lesion with diffuse loose myxomatous stroma containing fibrillar collagen and bland spindled to stellate-shaped cells (H&E, ×40).
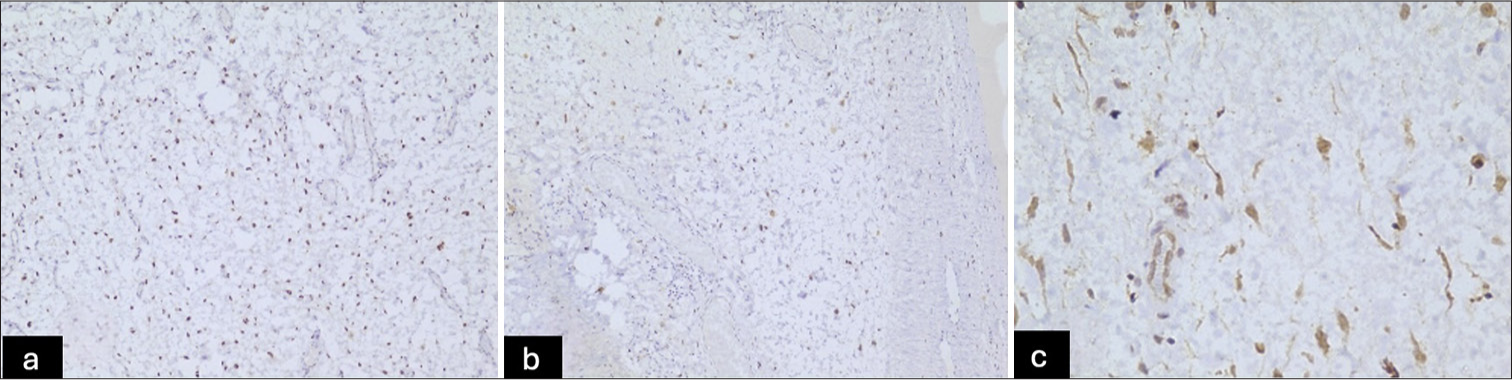
- (a-c) On immunohistochemistry, the tumor cells were positive for (a) estrogen receptor , 10X (b) progesterone receptor, 10X and (c) desmin, 20X.
DISCUSSION
Mesenchymal tumors in the lower female genital tract, especially the vulva, encompass a diverse range of neoplasms, including AAMs, slow-growing AM, angiomyofibroblastoma (AMFB), and cellular angiofibroma (CAF), among others. These tumors are characterized by stromal cells that are either spindle-shaped or epithelioid, interspersed with vascular elements, each with nuanced histological differences. Accurate diagnosis is crucial due to variations in clinical outcomes and treatment approaches. Superficial AM is mostly seen in middle-aged patients, and it can appear anywhere on the trunk and extremities. However, AAMs are specific to the perineal and pelvic regions. Deep AMs do not have a capsule and, have low mitotic activity, have a higher recurrence rate (~36–72%) after excision.2 These can be identified on computed tomography scans due to their distinct margin and lower density than muscle. On magnetic resonance imaging (MRI), they present as having a high signal intensity on T2-weighted images. This is likely due to their loose myxoid matrix and high water content. In addition, the myxoid tissue in the AM displays a laminated pattern with alternating hyper- and hypointense linear areas, which is caused by the presence of collagen fibrils.4,5 However, our patient did not undergo radiological investigation as the initial presentation resembled that of a benign mass.
Histopathologically, superficial AMs are present in the superficial tissue, are lobulated, and show only thin-walled vessels. Deep (aggressive) AMs infiltrate the deep tissue, present as diffuse growth rather than lobules, and show an admixture of both thin-walled vessels and thick-walled vessels. The current case showed features of deep AM, as evidenced by the deep infiltrative growth, non-lobulated sheets, and thin as well as thick-walled vessels within the growth. Positivity for ER and PR further supported the diagnosis of AM. AMFBs, while related to AAM, are clinically indolent and well-circumscribed, with alternating regions of hypo- and hypercellularity and spindle to epithelioid cells. Unlike AAMs, AMFBs rarely exhibit thick-walled vessels.6,7 CAFs, similarly benign, primarily affect the vulvovaginal region and have a low recurrence rate. Histologically, they feature spindle cells in a collagenized to hyalinized stroma, rather than myxoid stroma, with medium-sized vessels.8-10
Surgical excision is still considered the primary treatment for this medical condition. However, there are emerging hormonal therapies, such as GnRH agonists, that can be used as an alternative. Sun and Li reported a case study in which monthly injections of Triptorelin 3.75 mg were given for 3 months to prevent recurrence.11 Meanwhile, McCluggage et al. reported a case where Goserelin acetate 3.6 mg was administered once a month.12 However, the side effect profile of these drugs in the long-term and recurrence after discontinuation makes them difficult to establish as first-line therapy. Schwartz et al. published a case report on recurrent AAM where they used aromatase inhibitors in postmenopausal females.13 Although benign, these tumors can recur due to incomplete surgical removal. Therefore, it is essential to ensure complete margin-free removal and to schedule routine follow-ups for at least 2 years post-surgery to detect any early recurrence and reduce the risk of complications.14 In our case, the asymptomatic growth was removed for cosmetic reasons, and no recurrence has been observed in the 1st year of follow-up. However, long-term follow-up is necessary for all patients due to potential late recurrences. Recurrence detection is best done using MRI.
CONCLUSION
Although AM is a benign tumor, its infiltrative potential and high local recurrence rate make it insidious. Wide local excision is still considered as the treatment of choice. It requires clinical or radiological follow-up. Adjuvant and neoadjuvant hormonal therapies are yet to be standardized.
Authors’ contributions
Dr(s) Charu Sharma and Rajiv Kumar had full access to all of the data in the study and take responsibility for the integrity and accuracy of the data. Study concept and design: Sharma C, Acquisition, analysis, and interpretation of data: Kumar R, Singh P, Shekhar S, Rao M and Patra S. Drafting of the manuscript: Kumar R and Sharma C. Critical revision of the manuscript for important intellectual content: Sharma C, Singh P. Shekar S.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.
References
- Aggressive angiomyxoma of the female pelvis and perineum. Report of nine cases of a distinctive type of gynecologic soft-tissue neoplasm. Am J Surg Pathol. 1983;7:463-75.
- [CrossRef] [PubMed] [Google Scholar]
- Aggressive angiomyxoma of the vulva: Which is the best management strategy? Description of a case report and review of literature of the last ten years. J Clin Med. 2023;12:1726.
- [CrossRef] [PubMed] [Google Scholar]
- Radiologic imaging findings of pelvic aggressive angiomyxoma correlated with surgical and pathological features. Egypt J Radiol Nucl Med. 2021;52:1-7.
- [CrossRef] [Google Scholar]
- Aggressive pelvic angiomyxoma and its mimics: Can imaging be the guiding light? Br J Radiol. 2020;93:20200255.
- [CrossRef] [PubMed] [Google Scholar]
- A benign neoplasm distinct from aggressive angiomyxoma. Am J Surg Pathol. 1992;16:373-82.
- [CrossRef] [PubMed] [Google Scholar]
- Vulvovaginal angiomyofibroblastomas: morphologic, immunohistochemical, and fluorescence in situ hybridization analysis for deletion of 13q14 region. Hum Pathol. 2014;45:1647-55.
- [CrossRef] [PubMed] [Google Scholar]
- Cellular angiofibroma: Clinicopathologic and immunohistochemical analysis of 51 cases. Am J Surg Pathol. 2004;28:1426-35.
- [CrossRef] [PubMed] [Google Scholar]
- Cellular angiofibroma and related fibromatous lesions of the vulva: Report of a series of cases with a morphological spectrum wider than previously described. Histopathology. 2004;45:360-8.
- [CrossRef] [PubMed] [Google Scholar]
- A tale of two vulvar angiomyxomas: Two cases and review of literature. Gynecol Oncol Rep. 2023;47:101204.
- [CrossRef] [PubMed] [Google Scholar]
- Aggressive angiomyxoma of the vulva: Case report and literature review. J Int Med Res. 2010;38:1547-52.
- [CrossRef] [PubMed] [Google Scholar]
- Aggressive angiomyxoma of the vulva: Dramatic response to gonadotropin-releasing hormone agonist therapy. Gynecol Oncol. 2006;100:623-5.
- [CrossRef] [PubMed] [Google Scholar]
- Hormonal therapy for aggressive angiomyxoma: A case report and proposed management algorithm. J Low Genit Tract Dis. 2014;18:E55-61.
- [CrossRef] [PubMed] [Google Scholar]
- Second recurrence of aggressive vulvar angiomyxoma: A case report. J Int Med Res. 2023;51:3000605231189366.
- [CrossRef] [PubMed] [Google Scholar]







