Translate this page into:
Standard operating procedure for running hair transplantation practice
*Corresponding author: Dr. C. Madura, MD, FRGUHS (Dermatosurgery), Medical Director and Chief Hair Transplant surgeon and Dermatosurgeon, Department of Dermatosurgery and Trichology, CUTIS Academy of Cutaneous Sciences, Bengaluru, Karnataka, India. maduradr@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Madura C, Mysore V, Garg A, Sattur SS, Dua K, Dua A, et al. Standard operating procedure for running hair transplantation practice. J Cutan Aesthet Surg. doi: 10.25259/JCAS_36_2024
Abstract
Hair transplantation involves a team of doctors, nurses, and technicians, and there can be constant change in team members which can pose a challenge to the operating surgeon. The standard operating procedure is documented step-by-step instructions for performing the tasks that achieve consistency, improve quality and safety, save time, and avoid missing any steps and knowledge loss. Standardizations of technique by following standard protocols will not only give consistent results but also enable smooth hassle-free surgery with automation.
Keywords
Standard operating procedure
Hair transplantation
Follicular unit extraction (FUE) guidelines
INTRODUCTION
Hair transplantation (HT) is a long surgical procedure involving a team of doctors, nurses, and technicians. There can be constant change in team members which can pose a challenge to the operating surgeon. Standard operating procedure (SOP) is documented step-by-step instructions for performing tasks that achieve consistency, improve quality and safety, save time, and avoid missing any steps and knowledge loss. Standardizations of technique by following standard protocols will not only give consistent results but also enable smooth hassle-free surgery with automation.
Preparation for transplant begins with patient selection and counseling and continues to pre-operative work-up, intra-operative period, and finally post-operative care. This article shares the SOP followed by authors from different practicing places [Flow Chart 1].
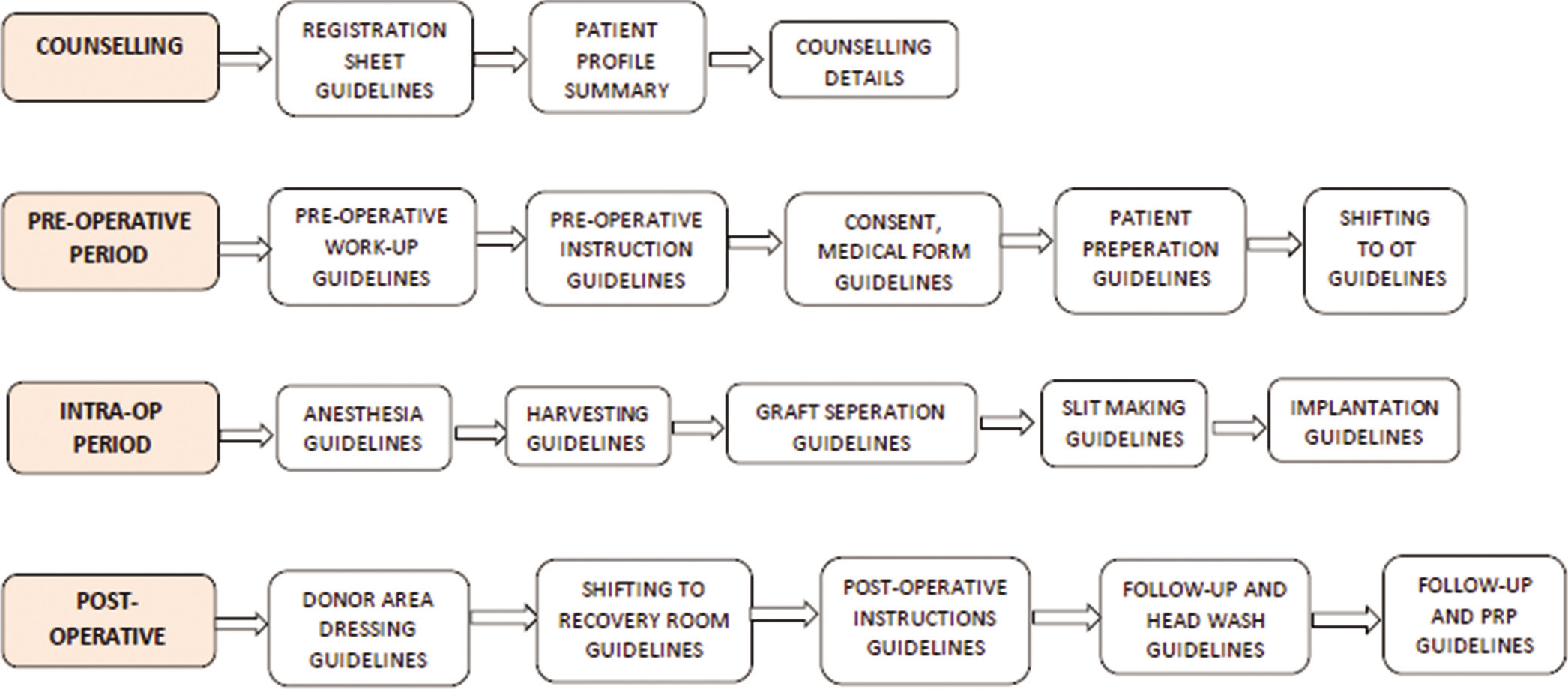
- Flow of events in hair transplantation and authors follow these guidelines as standard operating procedure.
SOP FOR PREREGISTRATION AND REGISTRATION
Patients can be given pre-designed questionnaire sheets by the receptionist during the waiting period before counseling which includes questions on knowledge of surgery, level of motivation, any fear factor, language preference, and expectation [Box 1]. This will assist the counselor in patient-oriented counseling.

- Registration sheet.
SOP FOR HISTORY TAKING AND EXAMINATION
A thorough history and examination is the basic mandatory step, which enables the physician to connect with the patient and helps him to customize the treatment plan.
Patient details – Name, age, gender, residence address, occupation, referring doctor.
Medical history, associated scalp diseases if any, comorbidities, allergies.
Treatment history including if using Minoxidil lotion currently/if had stopped in between, reason for stopping therapy/any previous procedures done for treatment of androgenetic alopecia (AGA).
Habits – Smoking, Alcohol consumption.
Any medications that the patient is taking – Aspirin, anti coagulants, including supplements such as fish oil, ginger, garlic, saw palmetto preparation, vitamin supplements.
Donor area – To check density and average thickness of hair in donor area. Rule out cause for shrinkage of donor area - Diffuse unpatterned alopecia (DUPA)/Reverse AGA.
Examining the scalp for the presence of scaling, folliculitis, tight scalp – Glidability and Laxity.
Record AGA grade and recipient area (Sites that concern the patient).
To understand and set right his/her realistic expectations
To know the timeline of patient, when he wants to get surgery done, fix tentative surgery date.
COUNSELING GUIDELINES
The main objective of counselling is to inform the patient about the steps of hair transplantation in simple words and to clear all the Doubts and misconceptions about the procedure.
Discuss different surgical options of HT.
Details about the follicular unit transplantation (FUT) and follicular unit extraction (FUE) technique to be explained using powerpoint presentation using simple terminologies such as strip method for FUT and dot method for FUE. The presentation includes a comparison of these two techniques in regard to the duration of procedure, scarring pattern, advantages, and disadvantages to make an informed decision about the choice of technique.
In addition, other details regarding the sequence of events in HT (pictures of marking/trimming of hair/post HT dressing), Post-operative (PO) sequence of events on days 0, 3, 7, and expected results must be discussed.
Draw planned hairline and discuss the customized plan and type of technique with the areas to be covered, with number of grafts needed, possible donor sites, and their appropriate recipient locations on the scalp.
Emphasize the importance of continuing the medical line of treatment to achieve and maintain good results.
PO instructions must be briefly discussed.
Provide a list of investigations and reference letter for fitness from physician/anesthetist.
Patient booked on email: all instructions are to be sent by email before booking.
SOP FOR PRE OPERATIVE EVALUATION
Fill history sheet
Examination findings including donor density, areas to be covered, number of grafts needed, number of grafts available in safe donor area, scalp examination for dermatological disorders
Vital records - Blood pressure, pulse rate and weight
Investigations preferably to be done at least 2 weeks before surgery - CBC: Complete blood count, RBS: Random blood sugar, HbA1C: Hemoglobin A1C, LFT: Liver function test, RFT: Renal function test, HIV: Human immunodeficiency virus, TSH: Thyroid-stimulating hormone, ECG: Electrocardiogram
Physician fitness for procedure - for all patients above 40, obese patients, and patients with comorbidities
Pre-operative instructions [Box 2]

- Pre-operative instructions.
PRE-OPERATIVE AND INTRA-OPERATIVE PATIENT PREPARATION
Patient file must be ready
Allot bed in pre-operative room, secure the patient tag, and provide a locker to the patient to keep all valuables.
Confirm if patient has eaten and taken all pre-operative medications
Explain entire procedure briefly
Consent form
Check vitals
Secure IV cannula
Test dose for lignocaine and if any IV antibiotics are advised
Administer pre-operative medication
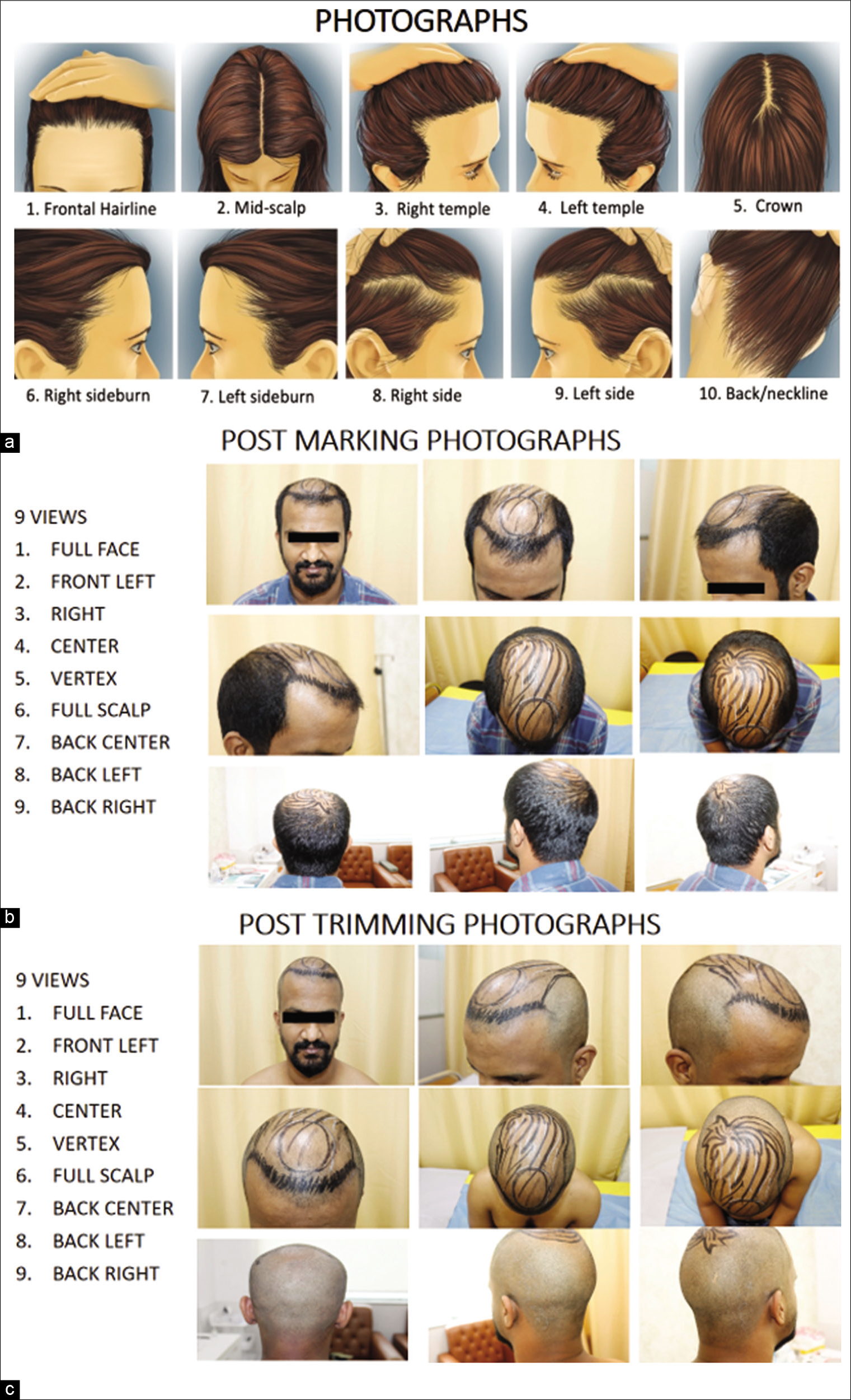
- (a), (b) and (c) Pre-operative and intra-operative patient preparation
Team introduction and instructions to patient
Introduce team of doctors, staff nurse, and technicians to patient
Inform the course of events and inform the role of surgeon, nurse, and technician - who does what
Approximate duration of the surgery, breaks between surgery, washroom, and water breaks as needed.
Reassure the patient on pain of surgery and also use pain distracting devices such as vibrators and playing music of the patient’s choice.
Inform positions during surgery and to keep moving lower limbs and before changing position not to get up suddenly.
The patient’s attender will be kept informed on the progress of surgery.
Marking and trimming
Confirm if marking photographs are done.
Technician to confirm trimming site and trimmer length before trimming the area.
Wash the scalp thoroughly using a surgical scrub, reinforce the markings with markers.
Post-trimming photographs to be taken
Consent to be signed after marking that the patient has approved the hairline design.
Document any additional points in the consent form by handwriting by the patient himself
Dawn the gown, mask, and foot cover before shifting into OT.
PAINTING AND DRAPING THE AREA
HT is a long surgery, and asepsis must be maintained. After marking and trimming, head wash is given with betadine scrub. Once a patient is shifted into the theatre, the staff nurse paints the scalp and forehead with betaine solution. Inform the patient to keep eyes closed and that betadine application will be cold to touch. Take care to avoid betadine dripping and accidental spillage into eyes and the markings should be preserved. Position the patient in a prone position for donor area harvesting and the patient’s ears should be covered with cotton swabs and gauze. Apply a sterile drape sheet around the neck. Betadine spray is done after every break.
ANESTHESIA GUIDELINES
Authors prefer to use 2% lignocaine with or without adrenaline with bupivacaine in 60:40 ratio for nerve blocks and infiltration solution, respectively. Use luer lock 3 cc syringes for nerve blocks and tumescent anesthesia and insulin syringes for infiltration [Box 3].
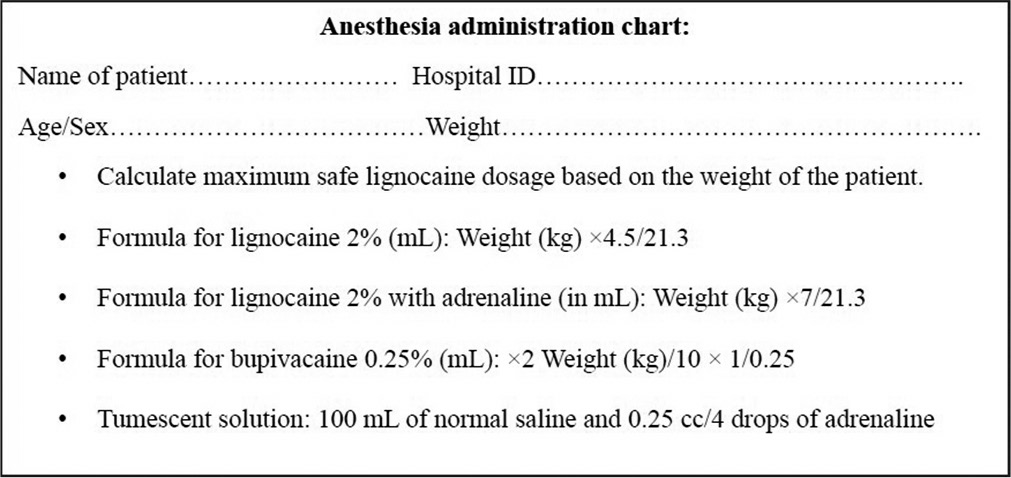
- Anesthesia administration chart.
Always use a vibrator device when the anesthesia is being administered.
Keep track of the amount of anesthesia being used for the donor and recipient area.
Keep the operating surgeon informed when the solution is about to finish.
Pulse oximeter or cardiac monitor should be attached. Check the vitals of the patient every 30 min.
Regularly keep refilling the syringes as and when required.
Write the consumed amount of anesthesia at the end of the surgery
HARVESTING GUIDELINES
Give proper position to the patient and look for doctors and assistant ergonomics.
Trolley 1 to place graft collection bowl with ringer lactate, anesthesia solutions, and extraction forceps.
Trolley 2 – to place only motorized punch machines with punches of different sizes and types.
Check for wire of the machine not to be entangled and foot switch should be in the vicinity.
Tumescent solution is injected in the deep dermal plane. Scoring to be done from distal to proximal row by row and targeted units are extracted, in a ratio of 1:4–1:5 leaving behind 4–5 units for every extracted unit
Use wet mop to gently wipe the bleeding. In case of excess bleeding, keep tumescent ready. Keep extra wet mops and tumescent-filled syringes ready.
Few of the first extracted grafts should be assessed for follicular length and assessed for thickness and quality. Note partial and total transection and also any missed grafts. In case of transection or capping, inform the operating surgeon so that punch size, depth, sharpness, speed, and torque can be adjusted accordingly.
Extraction to be done using traction on the one side. In case of lax scalp, counter traction may also be required. Inform if more transections/capping. Stop extraction if more transaction or capping and make adjustments
The technician performing extraction should follow all the rules of extraction without disturbing the scoring process.
2 forceps extraction is to be used, only if approved by the operating surgeon. Stop extraction if there is more transection/capping.
The extracted grafts should be immediately shifted to Ringer’s lactate bowl without letting them dehydrate. While transferring, follicles should not be crushed and handled carefully. Extracted grafts should be collected gently in the bowl, not on hand.
Thorough examination of all the grafts must be performed under microscope/magnifying loups before passing them for implantation.
Check the mops/gauze for entangled grafts before discarding them.
The coordination of the surgical team must be aligned in such a way that out-of-body time of the grafts is minimal and implantation of grafts must be performed in the sequence of extraction, i.e., first extracted grafts must be implanted first.
GRAFT HYDRATION AND SEGREGATION GUIDELINES
Chilling is not recommended with solutions with extracellular properties like ringers lactate or normal saline (NS) and room temperature is adequate
Doctor or technician should always use magnification during graft segregation and counting.
It is ideal to have a shallow tray filled with the holding solution and the graft segregation and counting is done in this tray with grafts immersed in the holding solution at all times. A sharp-pointed Jeweler’s forceps is used for this purpose as it precisely allows holding of the grafts with minimal trauma. Segregate and transfer the grafts into their respective chambers of the holding plate according to the time of harvest.
Enter the count on the sterile sheet (can be sterile glove cover) using sterile pen counting to be updated end of 1 h harvest
During implantation, Use continuous spray technique while grafts are being placed, when there is active bleeding obscuring the field, while fixing the grafts and on implanted areas.
RECIPIENT SITE GUIDELINES
SOP for slit making
Trolley to include implantation blades of needed sizes, anesthesia solutions, gentian violet
Check the marking of the recipient area, paint, and drape. Give anesthesia and wait for 7 min.
Meanwhile, check the graft length and fix the blade according to the length of the grafts.
Inject tumescent solution before slit making.
Dry mop should be used while making slits in the hairline. Wet mop to be used later to keep the area bloodless.
The assistant documenting the slits must update the operating surgeon after every 500 slits.
Appropriate density, depth, and direction of slits as per different zones of recipient area must always be kept in mind. Over-crowding of slits may lead to poor wound healing and necrosis.
After slits are made, stain with methylene blue/gentian violet and cleaned with wet mop. Shave the recipient area. Finally, flush with saline.
SOP for implantation
Implantation guidelines- forceps
Follow the plan of implantation on chart placed in operation theatre (OT)
To arrange up to 20 grafts on the hand at a time to supply for forceps implantation
Hold the grafts away from the bulge area. Avoid squeezing
Insert the graft in the direction of the slit, by root no touch technique
Do not let the grafts dry. Spray NS on the grafts once placed on scalp for implantation
Place grafts one by one without skipping the slits. Do not piggyback the grafts
Grafts should be fixed at the implanted site at the end of implantation. Only implantation forceps to be used for the fixing of grafts. While fixing, care should be taken not to bury/push the graft inside
Always scan the area to look for skipped sites, buried grafts, or grafts which pop out partially.
Implantation guidelines (implanters)
Graft loading trolly with grafts and implanters arranged separately according to size
Handle the grafts by holding only the epidermis with forceps and load into appropriate size implanters and loaded implanters to be immersed in holding solution/transferred for implantation,
Bulky grafts not to be loaded in implanters
Grafts should not pop out from the side slit of the implanter
Grafts must not be crushed nor allowed to dehydrate
Tumescent solution is injected before implanting grafts
The loading team is on right-hand side of the implanters.
Spraying guidelines
A 20 mL syringe with saline loaded with 26 gauge amputated needle. 5 areas to spray: (a) Grafts to implant, (b) area of implantation, (c) oozing area, (d) implanted grafts, and (e) arranged grafts on hand.
DRESSING GUIDELINES
Recipient site
NS spray clears bleeding spots during the fixation of grafts. Gentle pressure with wet gauze will stop bleeding points
After fixing, spray the implanted area with betadine solution (2 mL of betadine in 8 mL of NS) and then spray with NS
At the end of fixation, implanted area should be gently pressed with wet mop/gauze
Adjusting the grafts that were displaced due to movements on the scalp.
Donor area
Cleaning blood stains and povidone-iodine stains at the surgical site
Photographic documentation
Povidone-iodine ointment application over the donor area or Cuticell dressing
Steripad/absorbent dressing for dressing of the donor site and fixed with micropore tape
Surgical cap for patient (care to be taken that the cap is not touching the grafts)
Shifting the patient to recovery room accompanied by a technician and doctor.
MISCELLANEOUS
Vital monitoring guidelines
When connecting the blood pressure (BP) cuff and pulse oximeter, explain about the periodic inflation and deflation of BP cuff to the patient and also the beep sound
Record the baseline reading and every 1 hourly in the case sheet and regular monitor the parameters
Anesthetist to be called over when mean arterial pressure falls below 65 mmHg or above 100 mmHg or BP falls >20% of baseline reading
Do not disconnect the connector until patient sits for a while
Transient rise in heart rate is expected because of the adrenaline in local anesthesia injection.
Break guidelines
Inform patients about planned break times. Inform the patient to alert doctors if there is a need for restroom break or water break. To make limb movements before sitting upright.
All blood-stained mops are to be removed from the patient’s visual field.
Once the patient sits upright, clean all blood stains from the face.
Whenever taking a break in the middle of surgery, switch off the OT lights, make the patient sit, and inquire whether he is comfortable before he stands up. Keep a record of vitals and ask the patient if he/she is experiencing any dizziness. Remove BP cuff and pulse oximeter only once patient is stable.
Stand behind/support the patient throughout, in anticipation of any syncopal episode.
Instruct them not to lock the washroom, not to look in the mirror, and not to touch the area of surgery. Be in constant communication with the patient while they are using the washroom.
In charge, technicians should mandatorily accompany the patient. If patient is uncomfortable, doctor should be called immediately and put the patient in a comfortable position.
Once you shift the patient back, position the patient, connect the BP monitoring cuff, and ask the patient if he/she is comfortable.
Post-operative instructions
Discharge slip to be given to the patient documenting the procedure, duration, type of anesthesia, postoperative medication and instructions, contact number of doctor.
Travel arrangements for the patient should be discussed and done as needed.
Patient should be with an attender for the first night after surgery.
Patient to be admitted to hospital if patient has had any issues during surgery or if he has any comorbidities meriting monitoring in the opinion of the treating surgeon.
Emergency contact details must be highlighted and ask the patient to visit hospital immediately in case of pain/swelling/bleeding/itching/irritation/burning in the operated site.
Clear instructions about follow-up date and time must be given.
Reinforce to the patient that hair restoration is a delicate procedure and their adherence to the post-opt instructions is essential for optimal results.
Post-operative medications, special instructions on saline spray, diet instructions, position of sleeping, what to avoid, and be mindful on surgical site. Detailed instructions should be given to avoid any room for ambiguity.
Shampoo and cleaning
The transplant area
Hair should be washed 24–48 hrs after surgery. Inform the patient that we want the graft to adhere firmly during this time.
Wet your head with a bowl of room temperature water or with a gentle stream of water from the shower. If you use the shower, block the stream with your hand so that the water pressure is not too strong.
Lather up the shampoo in mug of little water and then with the palm of your hand, Pat this shampoo on the area gently (do not rub) wait for 1–2 min.
Gently rinse off with a bowl of water or a gentle stream of water from the shower.
Pat dry gently with towel. Do not rub the grafts to dry them.
After 7 days, you can begin to gently rub the grafts to help remove crusts.
After 10 days, you should be able to shampoo normally. However, scratching with nails should be avoided.
You can use any good-quality shampoo for hair washing.
A conditioner can be added to help in breaking down crusts.
SOP FOR SIMULTANEOUS HARVESTING AND IMPLANTATION BY MULTIPLE MEMBERS
Simultaneous extraction and implantation in scalp-to-scalp hair transplant
In the process of scalp-to-scalp simultaneous hair transplant, the extraction of donor hair follicles and their implantation into the recipient area occur concurrently. This innovative approach involves a coordinated effort between two teams, excising and implanting follicles simultaneously.
Team collaboration
Two specialized teams, one focusing on follicle excision and the other on implantation, work seamlessly together
The surgeon and assistant require minimal orientation to optimize their collaborative efforts.
Operative procedure
Both donor and recipient areas receive routine scalp anesthesia following established techniques and protocols.
The surgeon creates premade slits in the recipient area.
The patient assumes a comfortable position on a Thai massage chair, adopting the frog position.
FUE excision is performed by the surgeon, who may stand or sit based on personal preference.
A trained senior technician stands in front of the patient, conducting implantation using techniques such as implanters, no-touch to root stick, forceps, or other preferred methods.
As the surgeon excises follicles from one side of the donor area, the technician promptly checks and prepares the grafts for implantation.
Adjustments in speed between excision and implantation are made in real time to maintain synchronization.
Safety measures
The team remains vigilant for any signs of patient distress, including giddiness, sweating, or discomfort. Throughout the procedure, the team stays in verbal communication with the patient, addressing any concerns or issues promptly.
The patient is informed of the procedure and encouraged to communicate any discomfort or adjustments needed during the operation.
When the patient is in a standing position, precautions are taken to prevent vasovagal events, with the assistant positioned around the patient.
This refined approach to simultaneous extraction and implantation ensures efficiency, patient comfort, and a synchronized workflow, contributing to the success of scalp-to-scalp hair transplants.
Simultaneous scalp hair transplant on routine operating table
This procedure can be carried out using a routine surgical table or any operating table and involves two approaches:
Incremental excision and implantation
Grafts are excised in batches of 50–100, followed by immediate implantation
The patient remains on the operating table throughout the process.
Lateral positioning
The patient is placed in a lateral position with the head/implantation area over the edge of the head end of the operating table.
The surgeon conducts excision while either sitting or standing, adjusting position based on handedness and the donor area.
The implantation team is positioned on the head side of the patient, utilizing well-trained technicians or surgeons with implanters for efficient implantation.
Note: Care should be taken to avoid creating micro or macro irregularities and transition zone of the hairline as this may compromise hair direction and angle during simultaneous excision and implantation.
Simultaneous beard hair transplant to scalp
Operating table setup
Surgeon at operating table is ideal, allowing adjustment for the extension of the head end.
Neck extension silicone cushion or ring aids in extending the neck.
Patient positioning
The patient is placed in a neck extension position, with the scalp at the extreme head end of the operating table.
Local anesthesia is administered to the beard and neck, followed by the creation of premade slits.
Excision and implantation
The surgeon, standing on the side of the neck, performs excision, adjusting as needed for harvesting from the beard.
The implantation team stands on the head end, simultaneously implanting beard follicles using forceps/needles/or implanters.
Note: Difficulty may arise in simultaneously implanting the lowermost part of the crown (occipital side) in this position, so a part of the crown can be addressed in separate sessions of excision and implantation.
Simultaneous chest hair transplant to scalp
Patient positioning
The patient lies in a supine position on the operating table with a slight prop-up.
Local anesthesia is administered to the chest, and premade slits are created over the scalp donor area.
Simultaneous excision and implantation of chest hair follicles are facilitated by the supine position.
The surgeon does excision of chest donor hair follicles and same time supplies to assistant implanting in scalp recipient area premade slits. Chest hair follicles, being thinner and more sensitive to ischemia, contribute to improve outcomes when simultaneously excised and implanted.
These variations in positioning and techniques provide flexibility in simultaneous hair transplant procedures, ensuring adaptability to patient needs and optimizing surgical outcomes.
SOP FOR PERFORMING MULTIPLE SURGERIES
SOP multiple clinics
To do the surgery at multiple locations at the same time, a lot of homework is required to make sure that the patient gets quality hair transplant.
It involves the following steps:
Training of the team on both the surgical procedure and the software which will be used for documentation of the procedures.
Documentation on the day of surgery in the file as well as the software.
Setting up an audit team.
Training
To do the surgery in multiple locations at the same time, we need to train the team for around 3 months.
They should have an exposure of a minimum of 50 surgeries before doing the surgery independently.
During the training period, they should cover all the aspects of the surgery.
Along with the surgical steps, they need to be trained on proper documentation of the process being followed both in the hard copy format (i.e., the file) and the software.
The software helps us to standardize and document all the points starting from history taking to medical examination and the surgical steps.
The doctors as well as the supporting team should record all their training exercises in the log book.
Documentation of the surgical steps
On the day of surgery, all the documentation as mentioned by the other authors should be done on the software
The software should have the provision to record in detail the history, diagnosis, plan of the surgery, and the intra-operative steps (anesthesia, harvesting, slit making, and implantation).
There should be a provision for storing the pre-operative and post-operative pictures of the patient undergoing the surgery.
The doctor should check all the information put up on the software.
When the doctor is new, then the senior surgeon remains in regular touch with the doctor and keeps on following up with them.
In case, the surgeon feels stuck up during harvesting, he/she is asked to send the video of the procedure and the difficulty they are experiencing to the senior surgeon. The senior surgeon can then guide the consultant as to how to proceed by changing the parameters being used for harvesting.
Postoperatively, the clinic team should call up the patient as per the protocol of the clinic and the same call should be logged into the software.
The post-operative pictures should be uploaded in the software which can be evaluated by the audit team.
Audit
Once the surgery is done, and all the information is stored on the software, then the audit should be done.
The scope of the audit is to make sure that all the steps are done as per the prescribed guidelines. In harvesting, the number of grafts is matched, the graft transection rates are compared, and the time taken to complete the harvesting is noted. The out-of-body time for grafts is taken into account. In implantation, it is checked as to how much time it took to implant the grafts and whether any grafts were J shaped or not.
In any new clinic where the chances of deviation are high, one old team member is posted to make sure that all the protocols are being followed. The feedback by them is used to find the discrepancies.
If there are any discrepancies as compared to the normal, then a discussion is done with the doctor in charge to improve the quality of the procedure.
The post-operative calls are also checked through the software by the audit team.
A separate call is made by the head office directly to the patient to confirm whether the experience of the patient was up to the mark or not. This is also logged into the software.
If there is any negative remark by the patient, then the email discussion is started by the head office audit team to have a complete account of the patients’ procedure.
If it still remains unresolved, the discussion is done once a month with the treating doctor to iron out the experience of future patients.
In case, the result is not up to the mark and the patient is still unhappy despite the local surgeon meeting the patient, then the patient is made to meet the senior surgeon and if required the senior surgeon does the revision surgery.
LEARNING POINTS
SOPs make it easy to train new staff to overcome frequent attrition.
Following fixed protocols will not only avoid medico legal hassles but also reduces the learning curve and margin of error gets narrowed
Good quality of work simulates. It also helps in monitoring and fixing accountability.
CONCLUSION
Standardization of protocols leads to diligence and hence consistent results in HT. These protocols are by no means exhaustive and there can be other SOPs designed for all issues – managing emergencies such as syncope, bleeding, convulsions, sterilization protocols, Trolley preparation, position and ergonomics, cleaning protocols, and managing equipments.
Authors’ contributions
C Madura: concepts, design, definition of intellectual content, literature search, manuscript preparation, manuscript editing, manuscript review, Venkatram Mysore: literature search, manuscript editing, manuscript review, Anil Garg: manuscript preparation, manuscript review, Sandeep Suresh Sattur: Manuscript preparation, manuscript review, Kapil Dua: Manuscript preparation, manuscript review, Aman Dua: Manuscript editing, M Kamaresan: Manuscript editing, Mayank Singh: Manuscript editing, Venkatram Aniketh: Manuscript editing, Sukhbir Singh: Manuscript editing, BS Chandrashekar: Manuscript review. Sumit Agrawal :Manuscript editing.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.







